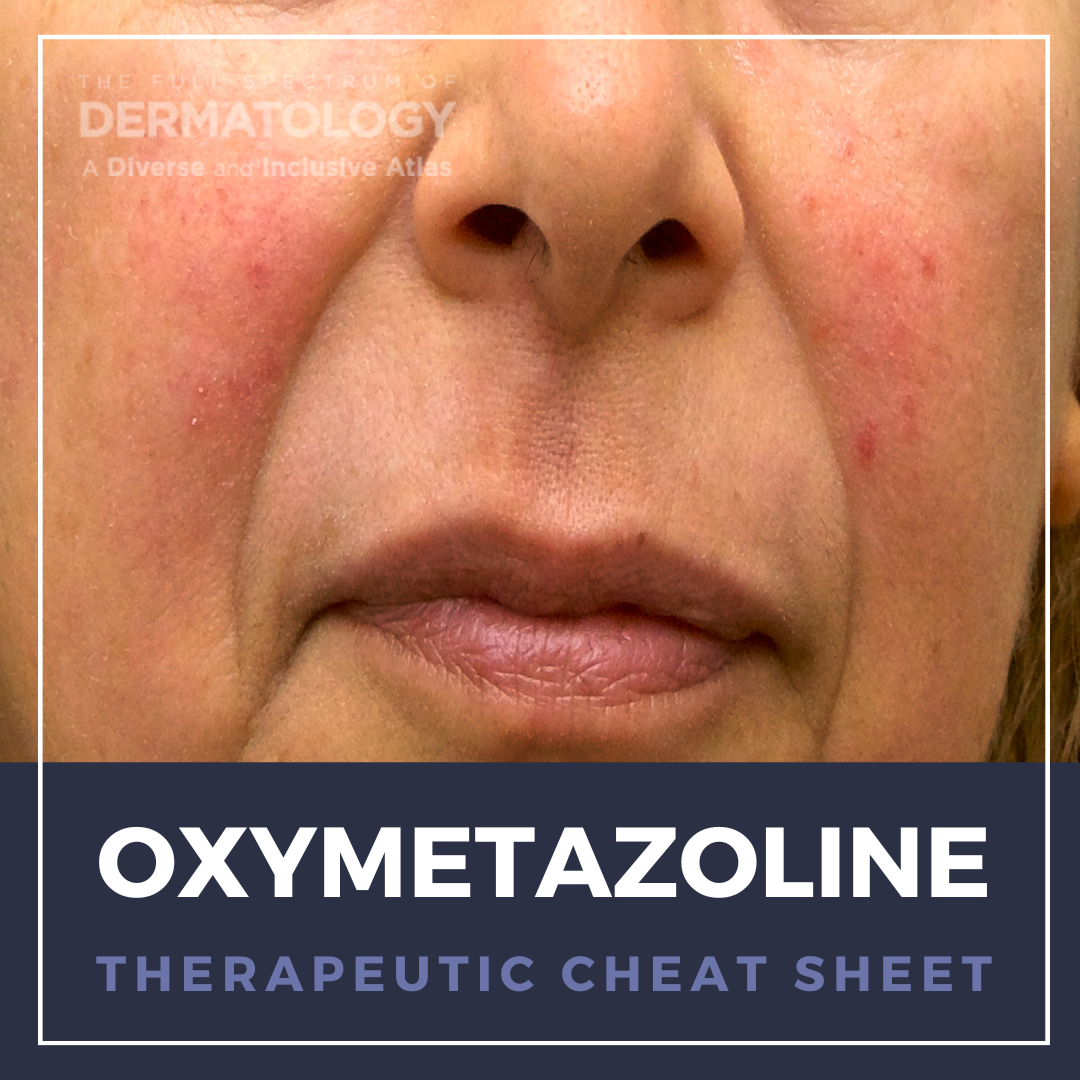
Oxymetazoline is an adrenoreceptor agonist which is FDA-approved for dermatologic conditions including persistent facial erythema in rosacea and blepharoptosis. Functioning primarily as a vasoconstrictor with additional anti-inflammatory properties, oxymetazoline targets the sustained vasodilated state of cutaneous blood vessels in rosacea by inducing vasoconstriction and reducing the persistent facial erythema. Additionally, as an adrenoreceptor agonist, oxymetazoline contracts the levator palpebrae muscle thereby lifting the upper eyelid and reducing ptosis. We continue our series, Therapeutic Cheat Sheet, with a closer look at oxymetazoline.
Oxymetazoline Therapeutic Cheat Sheet
Compiled by: Nidhi Shah, MD | Reviewed by: Adam Friedman, MD
TRADE NAME
-
- Rhofade (1% oxymetazoline hydrochloride cream)
- Upneeq (0.1% oxymetazoline hydrochloride ophthalmic solution)
MECHANISM OF ACTION
-
- Oxymetazoline is a selective ⍺1A adrenoreceptor agonist and partially selective ⍺2A adrenoreceptor agonist.1,2
- In rosacea, the superficial cutaneous blood vessels are in a sustained dilated state and respond to adrenergic stimuli. This response is primarily facilitated by ⍺1-adrenoreceptors and a subset of ⍺2-adrenoreceptors located post-syntactically on vascular smooth muscle cells. Activation of these postsynaptic adrenoreceptors results in cutaneous vasoconstriction and thereby reduced erythema.1,2
- Some evidence also suggests that oxymetazoline has anti-inflammatory effects such as reduction in pro-inflammatory cytokines and T-cell stimulation, regulation in arachidonic acid and arachidonic acid-derivative protein activity, and inhibition of respiratory burst activity. Additionally, ⍺-adrenoreceptor agonist treatments have been linked to reduced vascular endothelial growth factor expression resulting in inhibition of neovascularization.1
- As an ophthalmic solution, oxymetazoline activates the ⍺-adrenergic receptors on the levator palpebrae muscle (Mueller’s muscle) causing the muscle to contract and raise the upper eyelid.5
- *** Of note, in contrast to oxymetazoline, brimonidine is a highly selective ⍺2-adrenoreceptor agonist, which also leads to vasoconstriction; however, presence of presynaptic and endothelial cell ⍺2-adrenoreceptors may contribute to vasodilation and subsequent rebound erythema.3,4
FDA APPROVED FOR2,5
-
- Rhofade is approved for Persistent Facial Erythema (PFE) associated with rosacea in adults.
- Upneeq is approved for blepharoptosis.
OFF-LABEL DERMATOLOGIC USES6,7
-
- Rhofade has been used off-label for post-acne erythema and erythromelalgia of the knee.
DOSING
-
- Rhofade is for topical use only and patients should apply a pea-sized amount of cream to the affected area once daily, avoiding eyes and lips.1
- In both the REVEAL1 and REVEAL2 Phase 3 clinical trials, significantly greater proportions of patients treated with oxymetazoline vs. vehicle achieved at least a two-grade improvement in the Clinician Erythema Assessment (CEA) and Subject Self-assessment of Erythema (SSA) scores at 3-, 6-, 9-, and 12-hours post-treatment and response was maintained on day 29.2
- Upneeq is for ophthalmic use only and patients should instill one drop into one or both ptotic eyes once daily.5
- Studies demonstrated about 1 mm upper eyelid lift from Upneeq, with effects taking onset as early as 5 minutes post-instillation. Additionally, each dose was noted to be effective for about 6 hours, and this maintenance effect was visualized over 42 days of use.6
- Rhofade is for topical use only and patients should apply a pea-sized amount of cream to the affected area once daily, avoiding eyes and lips.1
WARNINGS AND PRECAUTIONS2,5
-
- Potential impacts on cardiovascular disease: As ⍺-adrenergic agonists may impact blood pressure, use with caution in patients with severe or uncontrolled cardiovascular disease, hypertension, and/or hypotension.
- Potentiation of vascular insufficiency: Use with caution in patients with cerebral or coronary insufficiency, Raynaud’s phenomenon, thromboangiitis obliterans, scleroderma, or Sjögren’s syndrome.
- There is an increased risk of angle closure glaucoma in patients with narrow angle glaucoma, and patients should seek immediate medical care if they develop signs and symptoms of acute angle closure glaucoma.
SIDE EFFECTS
Rhofade2-4,9-10
-
- Most common side effects include application site dermatitis, pain, paresthesia, and pruritus. Less common side effects include upper respiratory infection, headache, sinusitis, hypertension, and nasopharyngitis.
- In the clinical trial, about 3% of patients experienced worsening inflammatory lesions of rosacea, however, rebound erythema (recurrent erythema worse than baseline post-treatment or paradoxical erythema after application of medication) was noted in less than 1% of study participants. In contrast, 6.5% of patients experienced rebound erythema with brimonidine during the clinical trial, and 20% noted worsening of baseline erythema during post-marketing surveillance.
Upneeq5
-
- Most common side effects include punctate keratitis, conjunctival hyperemia, dry eye, blurred vision, instillation site pain, eye irritation, and headache.
DRUG INTERACTIONS2,5
-
- No direct drug interactions are noted; however, caution is advised when using in conjunction with beta-blockers, anti-hypertensives, cardiac glycosides, ⍺1 adrenergic receptor antagonists, and monoamine oxidase inhibitors as oxymetazoline may affect blood pressure and amine metabolism.
CONTRAINDICATIONS2,5
-
- None
PREGNANCY AND BREASTFEEDING2,5,10
-
- There is no available data on the use of Rhofade and/or Upneeq in pregnant women and no clinical data is available during lactation.
- Oxymetazoline 0.05% nasal spray is category C in pregnancy.
MONITORING
-
- None

FURTHER READING
If you would like to learn more about Oxymetazoline, check out the following articles in the Journal of Drugs in Dermatology:
Topical Oxymetazoline Cream 1.0% for Persistent Facial Erythema Associated With Rosacea: Pooled Analysis of the Two Phase 3, 29-Day, Randomized, Controlled REVEAL Trials, published in the Journal of Drugs in Dermatology
Stein-Gold L, Kircik L, Draelos ZD, et al
Abstract
Background: Rosacea is a chronic dermatologic condition with limited treatment options. Methods: Data were pooled from two identically designed phase 3 trials. Patients with moderate to severe persistent erythema of rosacea were randomized to receive oxymetazoline cream 1.0% or vehicle once daily for 29 days and were followed for 28 days posttreatment. The primary efficacy outcome was the proportion of patients with ≥2-grade improvement from baseline on both Clinician Erythema Assessment (CEA) and Subject Self-Assessment (SSA) at 3, 6, 9, and 12 hours postdose, day 29.
Results: The pooled population included 885 patients (78.8% female); 85.8% and 91.2% had moderate erythema based on CEA and SSA, respectively. The primary outcome was achieved by significantly more patients in the oxymetazoline than vehicle group (P<0.001). Individual CEA and SSA scores and reduction in facial erythema (digital image analysis) favored oxymetazoline over vehicle (P<0.001). The incidence of treatment-emergent adverse events was low (oxymetazoline, 16.4%; vehicle, 11.8%). No clinically relevant erythema worsening (based on CEA and SSA) was observed during the 28-day posttreatment follow-up period (oxymetazoline, 1.7%; vehicle, 0.6%).
Conclusion: Oxymetazoline effectively reduced moderate to severe persistent facial erythema of rosacea and was well tolerated.
J Drugs Dermatol. 2018;17(11):1201-1208.
Clinical Pharmacokinetics of Oxymetazoline Cream Following Topical Facial Administration for the Treatment of Erythema Associated With Rosacea, published in the Journal of Drugs in Dermatology
Kuang AW, DuBois J, Attar M, Ahluwalia G
Abstract
Background: Oxymetazoline cream 1.0% is FDA-approved for the topical treatment of persistent facial erythema associated with rosacea in adults. This phase 2, multicenter, randomized, double-blind, parallel-group study assessed the pharmacokinetics, safety, and tolerability of oxymetazoline in patients with moderate to severe erythema associated with rosacea.
Methods: Eligible patients were randomized to 1 of 8 treatment groups (oxymetazoline cream 0.5%, 1.0%, or 1.5% or vehicle applied topically either once or twice daily for 28 days). Pharmacokinetic analyses were conducted in patients receiving oxymetazoline. Plasma samples for pharmacokinetic assessments were collected prior to dosing and 6 times postdose on days 1 and 28.
Results: A total of 356 patients were included in the safety population (oxymetazoline, n=268; vehicle, n=88). Thirty patients (11.2%) in the oxymetazoline group reported treatment-related treatment-emergent adverse events, most of which were mild to moderate application-site reactions. Oxymetazoline, at all concentrations, was generally safe and well tolerated. Mean maximum observed plasma concentrations were ≤115 pg/mL across all groups; the highest mean values for area under the plasma concentration-time curve from time 0 to 24 hours following once- and twice-daily administration of oxymetazoline 1.5% were 1680 pg•h/mL and 2660 pg•h/mL, respectively. Systemic exposure to oxymetazoline increased dose proportionally with once- and twice-daily administration.
Conclusion: These findings support the use of oxymetazoline for the treatment of persistent facial erythema associated with rosacea.
J Drugs Dermatol. 2018;17(2):213-220.
REFERENCES
-
- Del Rosso JQ, Tanghetti E. Topical Oxymetazoline Hydrochloride Cream 1% for the Treatment of Persistent Facial Erythema of Rosacea in Adults: A Comprehensive Review of Current Evidence. J Clin Aesthet Dermatol. 2021;14(3):32-37.
- EPI Health, LLC. Drug label information. Rhofade—oxymetazoline hydrochloride cream. Updated May 9, 2023. https://dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=1ba1cc5b-4f7f-491b-a5af-a6a14fb5affd.
- Del Rosso JQ. Topical a-Agonist Therapy for Persistent Facial Erythema of Rosacea and the Addition of Oxmetazoline to the Treatment Armamentarium: Where Are We Now?. J Clin Aesthet Dermatol. 2017;10(7):28-32.
- Okwundu N, Cline A, Feldman SR. Difference in vasoconstrictors: oxymetazoline vs. brimonidine. J Dermatolog Treat. 2021;32(2):137-143. doi:10.1080/09546634.2019.1639606
- RVL Pharmaceuticals, Inc. Drug label information. Upneeq—oxymetazoline hydrochloride ophthalmic solution. Updated May 9, 2023. https://dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=e82b5788-a855-4165-a81f-7f15cb874612.
- Bacharach J, Wirta DL, Smyth-Medina R, et al. Rapid and Sustained Eyelid Elevation in Acquired Blepharoptosis with Oxymetazoline 0.1%: Randomized Phase 3 Trial Results. Clin Ophthalmol. 2021;15:2743-2751. Published 2021 Jun 25. doi:10.2147/OPTH.S306155
- Kalantari Y, Dadkhahfar S, Etesami I. Post-acne erythema treatment: A systematic review of the literature. J Cosmet Dermatol. 2022;21(4):1379-1392. doi:10.1111/jocd.14804
- Altemir A, Iglesias-Sancho M, Barrabés-Torrella C, Sanchez-Regaña M, Salleras-Redonnet M. Successful treatment of knee erythromelalgia with topical oxymetazoline. Clin Exp Dermatol. 2022;47(4):778-780. doi:10.1111/ced.15060
- Draelos ZD, Gold MH, Weiss RA, et al. Efficacy and safety of oxymetazoline cream 1.0% for treatment of persistent facial erythema associated with rosacea: Findings from the 52-week open label REVEAL trial. J Am Acad Dermatol. 2018;78(6):1156-1163. doi:10.1016/j.jaad.2018.01.027
- Roy K, Forman SB. Miscellaneous Topical Agents. In: Wolverton SE, ed. Comprehensive Dermatologic Drug Therapy. 4th ed. Elsevier; 2021:624-630.e3. ISBN 9780323612111.
Did you enjoy this Therapeutic Cheat Sheet? You can find more here.