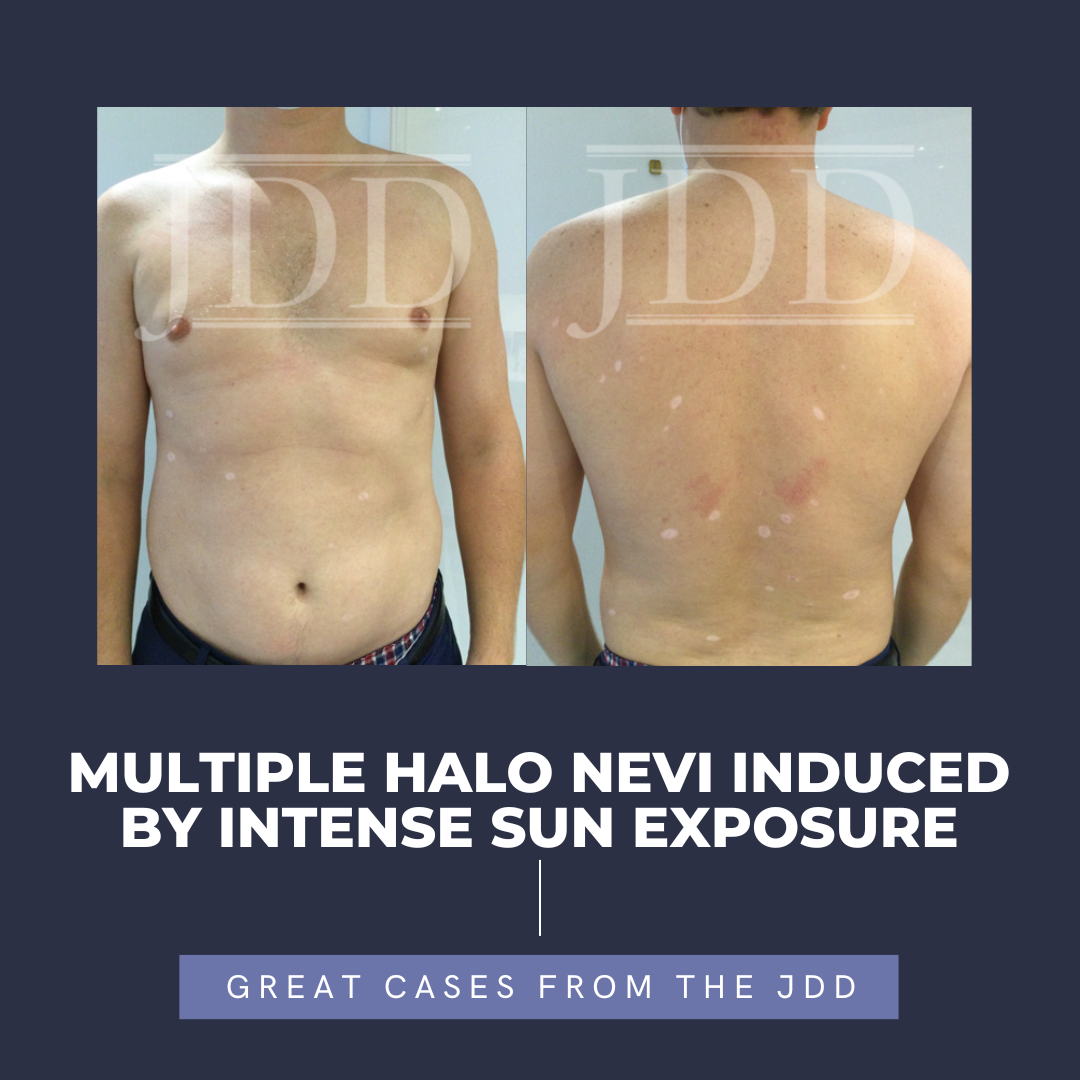
JDD authors present the case of a 38-year-old male who reported to their practice with multiple newly developed halos around 26 existing nevi on his trunk. The halo nevi developed after the patient, who lived in the northeast, spent 2 months on a lake in Alabama, with intense heat and sun exposure. This case is remarkable in that it points to ultraviolet exposure as one instigating factor in the development of halo nevi, the development of which is incompletely understood.
INTRODUCTION
Halo Nevi (HN) or Sutton’s nevi, are nevomelanocytic lesions surrounded by a ring of depigmentation. HN typically occur in adolescence and may affect 1% of the population.1 Sometimes they herald the disappearance of the nevus over time, and this process may take 10 years or longer.1 They have also been associated with the development of vitiligo and more rarely, with the development of melanoma in adults.2,3 Usually, HN will occur alone or in limited numbers, but there are rare cases of patients presenting with multiple lesions.4 We report the case of a 38-year-old male who presented to our practice with multiple newly developed halos around existing melanocytic nevi on his trunk. The halos began after the patient, who lived in the northeast, spent 2 months on a lake in Alabama, with intense heat and sun exposure. The phenomenon of multiple halo nevi developing after intermittent intense sun exposure has been previously reported in an adolescent Japanese male,4 but not in a Caucasian adult male, making this case rather unique and adding to the evidence that solar radiation is a contributing factor in the development of HN.
Clinical Findings
Our patient is a 38-year-old male who was born with blaschkoid pigmentation of the left lower extremity, extending from his L buttock to his lower leg. He had several common nevi on his trunk and returned to the office for yearly skin examinations. In September 2020, the patient presented after a summer vacation that included intermittent intense sun exposure with the congruent development of 26 HN distributed across his upper and lower back and abdomen. (Figure 1, 2).
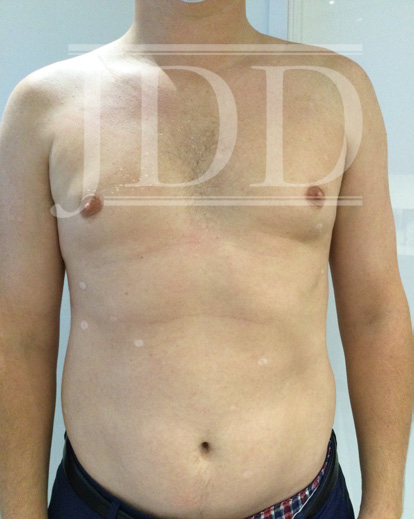
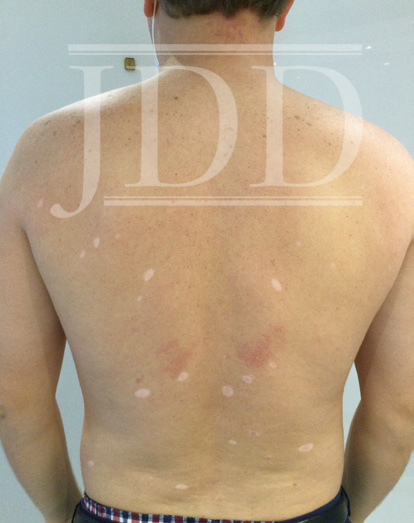
A complete skin examination was performed, and no atypical melanocytic lesions were notable. Our patient was advised to limit sun exposure, obtain an ophthalmologic examination, and monitor for new changes in the lesions at regular skin examinations. At his follow-up visit in January 2021, the HN were still visible and some of the nevi had further regressed leaving depigmented patches.
DISCUSSION
Researchers hypothesize that HN are created by the infiltration of acquired nevi by inflammatory cells, notably T lymphocytes that are CD8+ and Fox p3(+)/CD25+. It is thought that the Foxp3 (+) lymphocytes play a role in trying to decrease the number of cytotoxic CD8+ lymphocytes in the lesion, especially as they are increased in number at the early stages of HN development.5 The phenomenon of multiple HN has been seen in patients treated with checkpoint inhibitors for metastatic melanoma, eg, pembrolizumab, as reported in 2019, and ipilimumab.6,7,8 It has also been described in conjunction with medications such as interferon beta, infliximab, imatinib, and tocilizumab.9 Multiple HN may also be seen in genetic syndromes such as Turner’s syndrome, and associated with other autoimmune phenomena including thyroiditis and vitiligo.
A 2015 case report discussed the occurrence of 18 halo nevi in a 16-year-old male after a period of intense sunbathing. All nevi were excised and none were found to be abnormal, with immunohistochemistry demonstrating CD8+ T cell infiltration into the nevus. The authors suggest that the response may be the result of photo-koebnerization, or that UV radiation invokes an apoptotic pathway. Like the patient in their study, the halo phenomenon was not observed in every nevus in our patient, and it is unclear why some nevi were affected and others were not.4
CONCLUSION
6b75aa
REFERENCES
-
- Aouthmany M, Weinstein M, Zirwas MJ, et al. The natural history of Halo Nevi: a retrospective case series. J Am Acad Dermatol. 2012;67(4):582-6.
- van Geel N, Vandenhaute S, Speeckaert R, et al. Prognostic value and clinical significance of halo naevi regarding vitiligo. British Journal of Dermatology. 2011;164(4):743-9.
- Haynes D, Strunck JL, Said J, et al. Association between halo nevi and melanoma in adults: A multicenter retrospective case series. J Am Acad Dermatol. 2021 Apr;84(4):1164-6.
- Kawaguchi A, Yamamoto T, Okubo Y, et al. Multiple halo nevi subsequent to a short period of sunbathing. J Dermatol. 2015;42(5):543-4.
- Park HS, Jin SA, Choi YD, et al. Foxp3(+) regulatory T cells are increased in the early stages of halo nevi: clinicopathological features of 30 halo nevi. Dermatology. 2012;225(2):172-8.
- Nicolétis-Lombart I, Kervarrec T, Zaragoza J, et al. Multiple “halo nevi” occurring during pembrolizumab treatment for metastatic melanoma. Int J Dermatol. 2019;58(6):739-741.
- Alniemi DT, Fischer A, Greene LA, et al. Ipilimumab-associated halo-like inflammatory reactions around nevi during therapy for metastatic melanoma. Dermatol Online J. 2018;24(7).
- Plaquevent M, Greliak A, Pinard C, et al. Simultaneous long-lasting regression of multiple nevi and melanoma metastases after ipilimumab therapy. Melanoma Res. 2019 06;29(3):311-2.
- Kuet K, Goodfield M. Multiple halo naevi associated with tocilizumab. Clin Exp Dermatol. 2014;39(6):717-9.
- Brazzelli V, Larizza D, Martinetti M, et al. Halo nevus, rather than vitiligo, is a typical dermatologic finding of turner’s syndrome: clinical, genetic, and immunogenetic study in 72 patients. J Am Acad Dermatol. 2004;51(3):354-8.
Source
Loesch, Amanda J., Rebecca Kleinerman, and Ginger Lau. “Multiple Halo Nevi Induced by Intense Sun Exposure.” Journal of drugs in dermatology: JDD 22.12 (2023): e31-e32.
Adapted from original article for length and style.